For clinicians working in neuro rehabilitation, the question isn’t just how to help patients recover, it’s how to help them reclaim as much function and independence as possible. In recent years, activity-based therapy (ABT) has become a measurable component, and in many cases, a compelling alternative to traditional rehab models for neuro patients. Understanding the difference between the two shapes the care plans we build, the goals we set, and the outcomes we can realistically pursue for our patients.
The purpose of this blog is to give clinicians and therapists a clear overview of both approaches and to explore where activity-based therapy is opening new doors for patients with neurological and musculoskeletal conditions.
Traditional Rehabilitation: A Foundation Built on Compensatory Strategies
Traditional rehabilitation has long served as the standard of care for individuals recovering from injury, surgery, stroke, spinal cord injury, and a range of other conditions. Its core goals center on restoring function, preventing secondary complications, and teaching compensatory strategies that allow patients to navigate daily life despite deficits.
In traditional rehab, care plans typically include:
- Passive range-of-motion exercises and manual therapy
- Strengthening exercises focused on isolated muscle groups
- Functional mobility training with assistive devices
- Compensatory techniques to work around neurological deficits
- Patient education and caregiver training
These interventions are widely used across rehabilitation care and can be valuable for maintaining mobility, managing impairments, and supporting day to day function. However, traditionally, this approach has been rooted in a compensatory model, focused on helping individuals adapt to deficits rather than targeting the underlying neurological function. Activity-based therapy takes it a step further by targeting recovery at the neurological level by using intensive, task-specific practice to activate the nervous system, promote neuroplasticity, and support recovery that goes beyond compensation alone.
Activity-Based Therapy: Engaging the Nervous System’s Capacity for Change
Activity-based therapy (ABT) is built on the principle of neuroplasticity — the nervous system's remarkable ability to reorganize, adapt, and form new connections in response to meaningful, repetitive activity. Rather than working around deficits, ABT is designed to engage them directly.
ABT involves high-intensity, high-repetition, and task-specific movements that activate residual neural pathways, even in patients with spinal cord injuries, traumatic brain injuries, or chronic neurological conditions. The goal of this method is not just to help patients function despite their injury, but to also drive recovery at the neurological level.
Common ABT care plans include:
- Locomotor training with body-weight support systems
- Functional electrical stimulation (FES)
- Robot-Assisted Gait Training
- Exoskeleton-assisted gait training
- Task-specific upper extremity retraining
- Resistive cycling and neuromuscular re-education
The common thread across all ABT modalities is the deliberate, repeated activation of the sensorimotor system through purposeful movement. Rather than working around the nervous system's limitations, ABT works with its capacity for change, making it a meaningful option for patients where potential neurological recovery, not just functional compensation, is the goal.
Key Differences
While the two approaches are not mutually exclusive, understanding where they differ can meaningfully shape clinical decision-making:
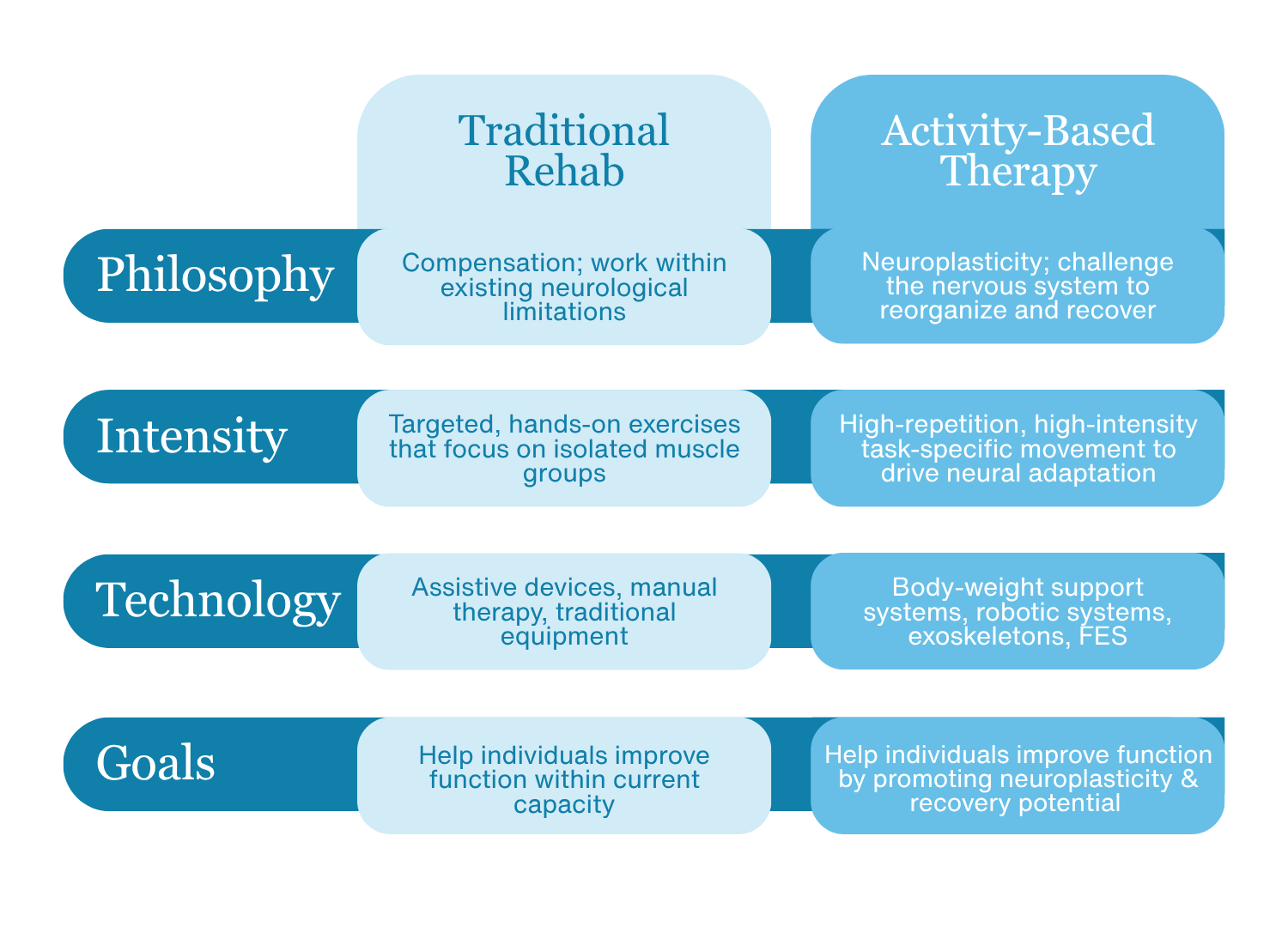
It's worth noting that this distinction isn't a critique of rehabilitation clinicians. In many settings, therapists are working within very real constraints, including insurance limitations, shortened lengths of stay, staffing demands, and the high acuity of patients in early recovery. At the same time, many individuals with neurological injury are not yet ready to fully engage in high-dose, task-specific training through conventional methods alone. Rehabilitation technologies can help bridge that gap, giving clinicians the tools to deliver ABT in a way that is safer, more efficient, and more accessible for patients.
The Evidence Behind Activity-Based Therapy
The research supporting ABT has grown substantially over the past two decades. Behrman and Harkema were among the first to document meaningful locomotor improvements through body-weight supported treadmill training in individuals with spinal cord injury, helping establish the clinical foundation for what would become a cornerstone of ABT. Since then, studies across patients with spinal cord injury, stroke, multiple sclerosis, and Parkinson’s disease have demonstrated great improvements in motor function, muscle activation, cardiovascular health, bone density, and quality of life following structured ABT programs.
Notably, some studies have reported motor improvements in patients with chronic, “stable” injuries - a population previously considered to have reached their recovery plateau. This challenges the long-held clinical assumption that neurological recovery is time-limited and reinforces the value of ongoing, intensive therapeutic engagement.
As with any evolving field, the evidence base continues to progress. Patient selection, injury type, therapy duration, and the specific ABT modalities used all influence outcomes. As with any clinical approach, individualized assessment remains the foundation.
Who is a Good Candidate for ABT?
ABT is not a replacement for traditional rehabilitation in all cases, but it offers particular promise for patients with:
- Incomplete/Complete Spinal Cord Injuries
- Stroke-related motor deficits, including chronic stroke
- Traumatic/Acquired brain injury with residual motor impairment
- Multiple sclerosis with gait and fatigue challenges
- Cerebral palsy and other pediatric neuromotor conditions
- Parkinson’s Disease
- Guillain-Barré Syndrome
The common thread is the presence of residual neural pathways that can be engaged through purposeful, high-repetition activity. Identifying those pathways is where clinical expertise comes in. A thorough clinical evaluation, including assessment of injury completeness, motor function, and patient goals, continues to be the foundation of any ABT program.
Two Approaches, One Goal: Building a Rehabilitation Plan That Does Both
The most effective rehabilitation programs don't force a choice between traditional rehab and ABT, they draw on both. Compensatory strategies help patients function safely in the near term; while ABT works to expand what's possible over time. When thoughtfully integrated, the two approaches can complement each other in ways that neither achieves alone.
At Healing Innovations, this integrative philosophy drives everything we do. We designed the Rise&Walk® InClinic to meet patients where they are, and help them reach further than they thought possible.
Curious about how activity-based therapy is being implemented in clinical settings? We’d love to show you! Whether you’re exploring options for your patients, your practice, or your facility, our team is happy to walk you through how the Rise&Walk can impact your patients' care in person or virtually.
Schedule a demo and see firsthand what’s possible when innovative therapy meets dedicated clinical expertise. Schedule a conversation with our team.




.png)
.png)
.png)
